Keeping the healthy part of the knee
Bad cartilage made walking too painful for Dawn Tatarka. Robotic surgery put her back on the dance floor.
Article Date:
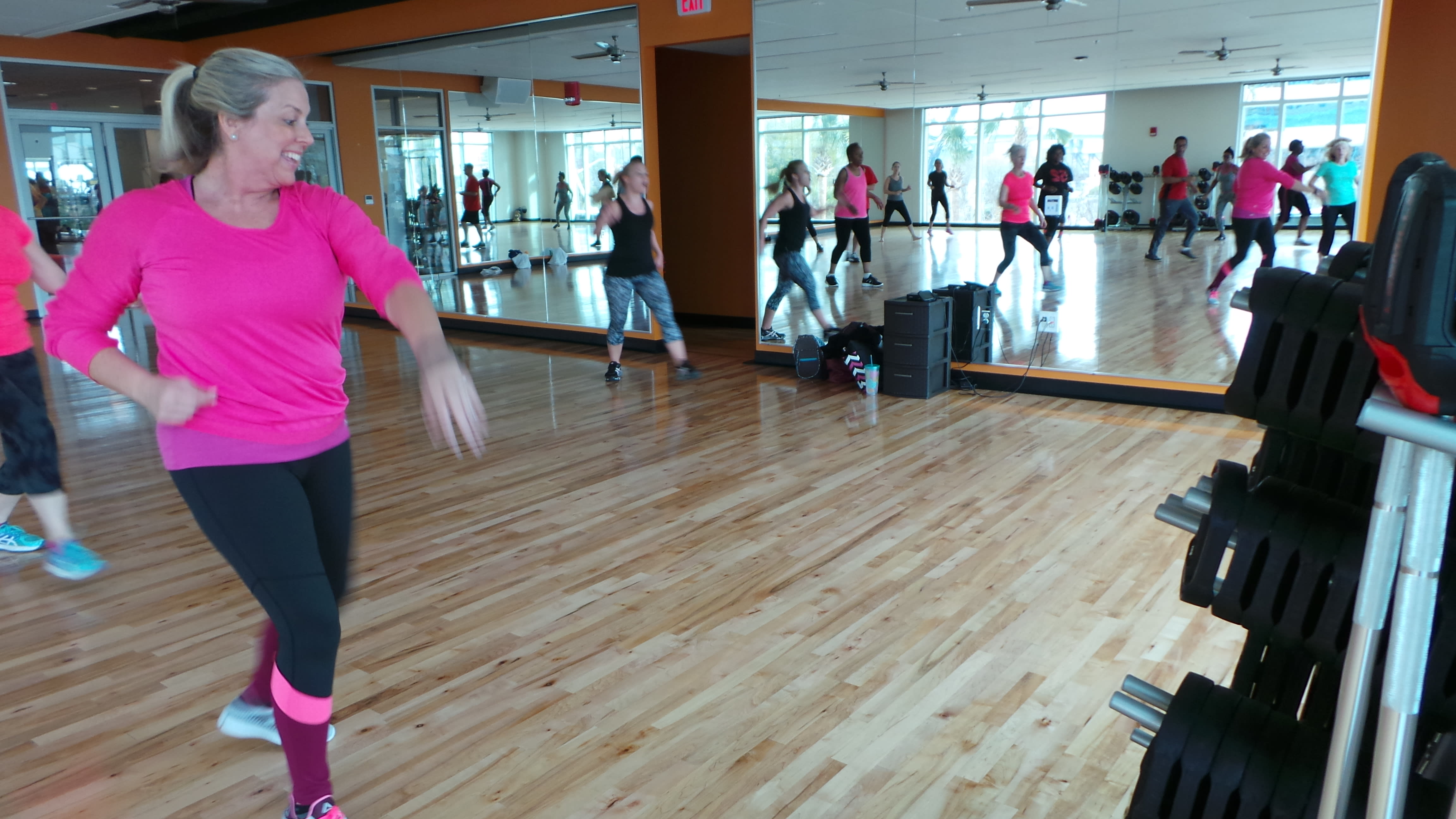
Moving to the sound of the beat, Dawn Tatarka raised her hands in the air, turned around and kicked her legs. She couldn’t stop smiling as she moved freely across the dance floor in the Zumba class at the Winston Family YMCA.
Tatarka has a lot to smile about. Just four years ago, she could barely walk and was in severe pain as the cartilage in her knees had degenerated from osteoarthritis.
With every excruciating step, she could hear the crunch in both knee caps as bone scraped against bone.
“I felt like I was 90, but I was only in my 40s. It was really bad,” said Tatarka, now 52.
Tatarka has always loved to dance, spending five days a week in Zumba and other high-energy dance classes for fun and exercise. The pain in her knees threatened to bring that part of her life to a halt.
“Over time, I had to wear knee braces to keep my knee caps in place and it became more and more painful,” Tatarka said. “Everything was a challenge. When you’re only 40, it makes it very difficult to lead a normal life.”
She couldn’t travel with her husband or enjoy time with her three sons. Walking up and down stairs became impossible, and she’d have to take elevators and escalators and avoid going places that required a lot of walking. Physical therapy, pain pills and cortisone shots provided no relief.
Then she found Steven M. Crenshaw, MD, an orthopaedic surgeon with Jacksonville Orthopaedic Institute who specializes in MAKOplasty® Partial Knee Resurfacing.
The procedure is for people with early-to mid-stage osteoarthritis, in which only the diseased portion of the knee is replaced, sparing healthy bone and ligaments.
The robotic-assisted surgery allows surgeons to be more precise in aligning and positioning the implants, which helps them last longer.
The minimally invasive procedure provides more rapid relief from pain, a shorter hospital stay, a quicker return to daily activities and more natural knee function.
Using the system’s software, doctors use a CT scan to create a 3D model of the patient’s knee. From this model, a pre-surgical plan is developed for the positioning of implants based on the patient’s unique anatomy.
The procedure “can significantly improve the quality of life for patients whose osteoarthritis is not advanced enough for a total knee replacement but whose pain can no longer be controlled by medication and other non-surgical options," said Dr. Crenshaw, who was the first orthopaedic surgeon trained and certified in the procedure at Baptist Medical Center Jacksonville
Tatarka’s surgery was performed in January 2013, followed by rehab at the hospital’s Joint Center.
Tatarka, who also took dance and ballet classes as a child, had both knees repaired at the same time. Within a few months, she was back dancing.
“For me, MAKOplasty was a very good solution for what was ailing me with my knees,” Tatarka said. “MAKOplasty is so precise. They kept the good part of my knee and only replaced the diseased tissue.”
Two year after her surgery, she celebrated her 50th birthday with a 10-day family trip to France, including time in Paris walking more than 20,000 steps each day.
“I would have never been able to walk that if I didn’t have my knees repaired. I was determined to get back to a normal walking life style and travel,” she said.
She’s also back to her normal routine with her children, which includes taking her youngest to school baseball games and games with his travel team. She also enjoys babysitting her 2-month old granddaughter.
And she’s back to dancing, joining various classes in the area.
“It’s absolutely a blast,” she said. “Dancing takes your mind off everything else.”



