'Why not me?’
25-year-old makes hole-in-one only weeks after awake brain surgery.
Article Author: Wesley Roberts
Article Date:

Bender Middlekauff was dozing off on his sofa when he had what he describes as a "vocalized, out-of-body experience." His eyes rolled back in his head and he fell to the ground. Knowing immediately something was wrong, his friend, Hunter, reacted quickly and called 911.
The paramedics rushed Middlekauff to the Emergency Center at Baptist Medical Center Beaches, where his parents met him. Initially, the Middlekauffs thought Bender's seizure was related to a dirt bike accident years earlier.
He spent the night in the Emergency Center while the team ran numerous tests, including a CT scan and MRI.
"We were waiting to be discharged from the hospital on Tuesday, March 10, 2020, so I could return to my normal, simple life," explained Middlekauff. "The day took a dramatic turn."
A rare brain tumor diagnosis
Middlekauff's MRI revealed he had a brain tumor.
Casey Carrigan, MD, a former neurohospitalist at Baptist Health, told Middlekauff the tumor was suggestive of a slow-growing type of brain tumor called an oligodendroglioma, which can eventually lead to seizures, but the type of cancer would need to be confirmed during surgery.
Middlekauff's mind swarmed with confusion and questions.
"This diagnosis would change my life forever," he said.
Dr. Carrigan referred Middlekauff to Robert Cavaliere, MD, neuro-oncologist with Baptist MD Anderson Cancer Center, and Eric Sauvageau, MD, neurosurgeon with Lyerly Neurosurgery, an affiliate of Baptist Health.
Dr. Cavaliere explained that an oligodendroglioma is a rare brain tumor that occurs most often in men between the ages of 35 and 44. Only about 1,000 people receive this diagnosis each year.
"Thankfully my city of Jacksonville is home to some of the best doctors in the world," said Middlekauff. "After several follow-up meetings and consultations, it was determined, without a doubt, that surgery was necessary."
Before the procedure, Middlekauff did his homework.
"Bender has always had an inquisitive mind, and he did an extensive amount of research about his diagnosis," explained his mother, Dina. "Dr. Sauvageau answered so many questions for Bender so he knew the ins and outs of every detail of his surgical experience."
Opting for an awake craniotomy
Middlekauff's tumor was located in close proximity to the left frontal lobe, the area of the brain linked to speech production and function on the right side of the body.
After much research, Middlekauff opted for an awake craniotomy, meaning he would be conscious and talking during the brain surgery, allowing Dr. Sauvageau to be more aggressive in the removal of the tumor.
"The brain is quite eloquent. While we know where certain functions are generally located, below the surface, we're not always able to pinpoint exact areas that affect language, speech and other motor skills prior to surgery," said Dr. Sauvageau. "Bender was young and a great candidate for an awake craniotomy. We would be able to assess in real-time to make sure we were not impacting important functions of the brain during the removal of the tumor."
The surgery was scheduled for March 26, 2020, with Dr. Sauvageau, whose mutual connection with the family brought extra comfort to the Middlekauffs. Dr. Sauvageau's daughters attend school where Dina is a second-grade teacher.
To avoid delay of the surgery due to the rise of COVID-19 in Florida, Dr. Sauvageau contacted Middlekauff on March 19 to see if he could undergo surgery the following day at Baptist Medical Center Jacksonville. Middlekauff agreed.
The morning of surgery, Middlekauff was joined at the hospital by his mother, while his siblings and father waited at home, due to limited visitation during the pandemic. In pre-op, Margaret Blincow, BSN, a nurse in the neurosurgical operating room, walked in to meet Middlekauff.
"I immediately recognized her name tag," said Middlekauff, recounting that having her as part of his care team made him feel even more at ease on the day of surgery. "Margaret was a mutual friend of my sister, Carlton." Blincow knew that one of the things she could do to ease Middlekauff's nerves before the operation was to play whatever music he recommended as he was rolled into the operating room.
"He requested anything southern rock, so I ran to put the station on shuffle before he came into the OR," Blincow said.
As Middlekauff was pushed into the operating room, the Lynyrd Skynyrd song "Sweet Home Alabama" was playing through the speakers.
"At first I thought Margaret put this song on specifically," said Middlekauff, a University of Alabama graduate. "This song was one I listened to throughout my years growing up as an Alabama fan, and hundreds of times while I was in school. When I found out this song just happened to be playing, I knew it was a 'God nod.'"
Talking during surgery
Middlekauff's awake craniotomy required a team approach led by both the neurosurgeon, Dr. Sauvageau, and the neuro-anesthesiologist, Miguel Bejar, MD.
"Bender would be playing an active and critical role in his surgery. He was initially asleep while the incision was made and the skull was opened," explained Dr. Bejar. "Then he was awake to talk and complete other verbal tasks to assess the impact on neurological function as the tumor was removed."
"Once he was awake, my job was to keep Bender talking, constantly," said Blincow, who held his right hand the whole time. "If Bender paused or stopped talking, Dr. Sauvageau would say, 'Bender, Bender, can you hear me? Keep talking to Margaret.'"
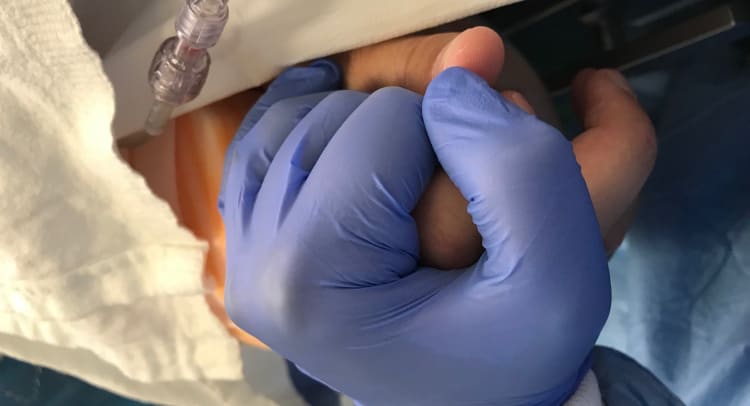
Blincow said keeping Middlekauff talking was easy at first, but she had to get creative to keep him talking for five hours straight.
"We talked about everything from his childhood to his first hole-in-one on the golf course. He recited the days of the week, the months of the year, inspirational quotes from Pinterest, the Pledge of Allegiance, and the Lord's Prayer."
During surgery, Blincow even helped Middlekauff FaceTime with his mother, who was in the waiting room, for 50 minutes! His mom wrote about the experience, "It was only through the power of the Holy Spirit and all the prayers lifting us up that I could focus and speak to my precious boy while I could see the brain surgery being performed behind the plastic above his head! Intense is an understatement."
Bender had an intraoperative MRI (iMRI), allowing images of his brain to be generated in real-time in the operating room during surgery. The iMRI helped confirm the removal of the tumor was successful, and no additional resection was needed.
Staying strong in recovery
Following surgery, Middlekauff was taken to the Neurocritical Intensive Care Unit for recovery, and with restricted visitation due to COVID-19, he had to FaceTime with his family rather than having in-person visitors.
"It was incredible to see his smiling face and hear him speaking to me. We both got a little teary when he could not answer all my questions because of a delay in his speech," wrote Dina. "Even though we had been warned that this was temporary and very normal, it was scary for Bender and upsetting for me. When we had to hang up, he said 'Stay strong,' once again proving his courage and strong character."
Dr. Sauvageau called Middlekauff's family the next day and explained that he was doing really well, and "his MRI was pristine." He was confident the tumor was removed entirely.
After two nights in the hospital, Middlekauff's family was ecstatic to spend time with him at home.
Back on course
As expected, Middlekauff's speech was delayed following surgery, but practice and constant talking would help it return to normal. However, his intelligent mind wasn't slowing down. A civil engineer, Middlekauff practiced physics problems the night he arrived home from the hospital.

"I couldn't talk very well at that point, but I could write, and doing physics problems would continue to exercise my brain," he recalled.
His family took the "Keep Bender talking" task head-on. They went through photo albums to name family members and objects, practiced worksheets from his nurses, FaceTimed with family and friends – anything they could think of to keep him talking!
In the days and weeks after the surgery, he was itching to get back out on the golf course. Two weeks after surgery, he asked Dr. Sauvageau if he was cleared to play. Dr. Sauvageau agreed he could get back out on the course, but jokingly made him promise no more hole-in-ones after hearing all about Middlekauff's first hole-in-one during his surgery.
Just six weeks after surgery, Middlekauff hit his second hole-in-one.
The reroute
Though a follow-up MRI confirmed the "all clear," Middlekauff will move forward with post-surgery cancer treatment options including proton radiation therapy and chemotherapy. He is receiving proton therapy treatment at the UF Health Proton Therapy Institute, followed by chemotherapy with Dr. Cavaliere at Baptist MD Anderson.
This experience has changed the course of his life dramatically, what Middlekauff has referred to as God putting his life's GPS on a "reroute," but he has leaned on his faith and the support of his community and loving family.
Middlekauff recently wrote: "God would never lead me to undertake something without first equipping me for the task, so instead of feeling sorry for myself and thinking 'Why me?' I have started to ask the question 'Why not me?'"
Learn more about neuro-oncology treatment options
The Neuro-Oncology Clinic at Baptist MD Anderson Cancer Center uses the latest technology and treatments, including aggressive treatments, targeted therapies, and less-invasive treatment options.
Story last updated: April 5, 2023



