Continuing COVID complications
Young father is among growing number of long-haulers.
Article Date:
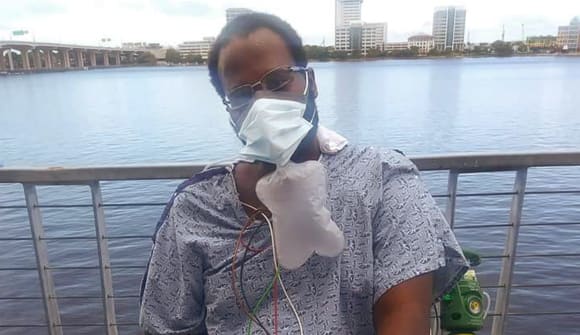
Intense chest pressure, extreme fatigue and labored breathing.
Difficulty getting up off the couch. Supplemental oxygen.
This is the new normal for Kaven Wright, a 34-year-old Jacksonville native who was discharged from Baptist Medical Center Jacksonville on September 15, 2020, after more than eight weeks in the Intensive Care Unit (ICU) battling COVID-19. Nearly three months into his recovery, the once-healthy and active father is still riding a corona-coaster, of sorts.
Puzzling phenomenon
Nearly a year after the coronavirus pandemic began, doctors and patients are just beginning to learn the long-term effects of COVID-19.
Some patients, dubbed “coronavirus long-haulers,” struggle with persistent symptoms lasting more than eight weeks and spanning multiple organ systems. There are no statistics yet as to how prevalent the phenomenon really is, but the COVID Symptom Study – a United Kingdom-based COVID-19 research initiative – estimates one in 20 people who get COVID-19 become long-haulers.
“I survived being on the ventilator for 40 days and even learned to walk again,” said Wright. “So when I was cleared to go home, I thought I would continue recovering. I’ve been so fatigued and weak that I’ve spent most of my time on the couch or in the recliner. I need help from my brother or the support of armrests to stand up, and I use a cane when I walk. Most surprising to me, though, is the numbness and tingling in my feet due to nerve damage.”
A spectrum of symptoms
As shocking as Wright’s story is, he is not alone. Many COVID survivors are showing signs of damage to multiple organs and experiencing lingering symptoms months after initial recovery.
“We are seeing a variety of different patterns starting to arise with patients who have initially recovered from COVID-19,” said pulmonologist Juan D. Pulido, MD, director of Critical Care at Baptist Medical Center Beaches. “The long-term effects we are dealing with are not only specific to lung damage and inflammation, but also psychological and neurological problems. We’ve also had to use a variety of different medications when treating COVID patients, all of which can cause a range of side effects.”
Some of the lingering symptoms long-haulers have reported include:
- Erratic heart rate
- Severe fatigue
- Cognitive issues such as brain fog and memory lapses
- Shortness of breath
- Blood pressure fluctuation
- Loss of taste or smell
- Dizziness
- Hair loss
Who is more at risk?
Older people and those who have had a severe case of COVID are most likely to experience long-term complications after initial recovery, but even patients who had mild to relatively moderate symptoms are reporting lingering effects.
Using data from the COVID Symptom Study, researchers at King’s College London identified characteristics of people most likely to develop long COVID:
- Age (over 65)
- Obesity
- Sex (women)
- History of asthma
- High number of symptoms during the first week of infection
For patients who have underlying lung disease, like Wright, who has a history of asthma, COVID can cause an overall worsening of the condition due to inflammation of the respiratory system.
Determining vulnerability
Now in the peak of a third wave of infections, research from the first and second waves suggests lung damage may explain some of the symptoms some long-haulers experience.
“We do a complete pulmonary function test after our COVID patients are discharged and during follow-up exams in the clinic to assess their new function and baseline,” said Dr. Pulido. “What we’ve seen affected most is the ability to get oxygen in and carbon dioxide out. Coronavirus causes inflammation and triggers cellular damage in the lungs, which can impair normal function and lead to long-term breathing problems. That is why some patients can still be symptomatic and short of breath despite testing negative for the virus.”
Dr. Pulido said COVID can also cause parts of the immune system to become overactive, triggering harmful inflammation throughout the body (not just the lungs). So, it really depends on the degree of inflammation and how the patient’s body responds to determine who’s more vulnerable to long-term symptoms and who quickly recovers.
“In some cases, we’ve seen it take as long as three or four months before patients start to feel like they’re back to normal,” said Dr. Pulido. “The inflammation specific to COVID tends to last longer than inflammation from influenza or a bacterial type of lung infection.”
The road to recovery
Today, Wright is focused on healing so he can play with his son again and hopefully return to work early next year. He continues to pace himself on his road to recovery and works closely with his primary care physician on a regimen to help strengthen his immune system.
“I’ve gone from zinc to elderberry to Vitamin C – you name it,” said Wright. “I also try to walk as much as I can, but I know to take it easy if I see my blood oxygen levels go down on my pulse oximeter. I never want to experience what I went through with COVID again and just want to get back to my old self.”
“COVID is a moving target – we’re constantly learning new information – so our approach today might be totally different than a week or two from now,” said Dr. Pulido. “I can’t emphasize enough the importance of a healthy lifestyle, which includes a well-balanced diet and exercise with safe outdoor exposure. We are starting to recommend supplemental vitamin D and C to help boost the immune system, especially for people who are not getting enough safe sun exposure or eating a well-balanced diet. Try taking a light stroll around the neighborhood for some fresh air and activity, and getting adequate sleep to help your immune system rebuild.”
At Baptist Health, we want to help keep our community informed about COVID-19. For more information, visit baptistjax.com/covid19 or wolfsonchildrens.com/covid19.
Baptist Health physicians are here for you during this time and can diagnose, treat and prescribe medications virtually. Request an online doctor appointment here.
Source: COVID Symptom Study App